Is Innovation Possible While Balancing Quality and Patient Safety?

Innovation drives the discussion in healthcare today. It holds enormous potential to drive down costs while improving healthcare. It might even save some struggling healthcare institutions while better serving patients. In fact, two-thirds of healthcare leaders and clinicians agree that hospitals and health systems are in need of disruptive innovation. However, that can be accomplished only if the innovation meets the very high bar of three core objectives:
- Patient and provider adoption
- Cost-effectiveness
- Safety, security, and trust
That’s the problem with most of the innovation floating around healthcare today.
It’s developed without an in-depth understanding of the inner workings of healthcare. Innovative disruption may be needed, and it may come from external start-ups, but to affect real and lasting change it must incorporate the following:
- A refinement of internal processes and identification of internal challenges
- Breakthrough discoveries and disruptive solutions that address those specific challenges
- The ability to change behaviors that affect outcomes is understood and incorporated into the implementation
That brings us to the seminal question – is there any scenario in which patient safety, quality of care and innovation can be successfully married?
What is disruptive innovation?
To answer that, we must first define disruptive innovation. It’s not what you think it is. One of the world’s top experts in the field, Harvard Business School professor Clayton Christensen says that disruptive innovations are not breakthrough technologies. Instead, they make products and services “more accessible and more affordable, thereby making them available to a larger population.” Perfect- that’s exactly what healthcare needs today.
Christensen says that disruptive innovation is a process by which “a product or service initially takes root in simple applications at the bottom of a market—typically by being less expensive and more accessible—and then relentlessly moves upmarket, eventually displacing established competitors.” Simple is better. Let’s look at what’s happening with disruptive innovation in healthcare today. You’ll see that the most successful innovations are exactly that – surprisingly simple.
Thinking about change, and learning, and quality
There are those who would say that innovation managed by large quasi-governmental institutions is an oxy-moron of the highest degree. The reality is that healthcare and high-tech must collaborate to develop solutions that reduce risk while improving quality and safety.
Case in point: The Agency for Healthcare Research and Quality (AHRQ) and the Institute for Healthcare Improvement (IHI) are two agencies leading the charge to encourage high tech/healthcare collaboration. They know that for innovation to occur, it must first pass the litmus test of a realistic application on the front lines of healthcare.
The Agency for Healthcare Research and Quality (AHRQ) gathered healthcare professionals together beginning in 2012. Their goal was to “adapt and implement innovations” to their quality improvement needs. In other words, they looked at new ideas to see if they could improve quality in the working world of hospitals and health systems. The AHRQ’s “Learning Communities” focused on three healthcare delivery challenges:
- Reducing Non-Urgent Emergency Services
- Promoting Medication Therapy Management for At-Risk Populations
PPFC offers a good example of tiny changes with not-so-tiny impact. It discovered that offering patients and their families the use of notepads increased the rate at which patients asked questions of their providers. University of Michigan Health System, UC Irvine Health, and Northwestern Memorial Hospital implemented the notepad in small steps; a few units at a time. Most noteworthy is that they found it resulted in significant improvements in quality:
- Hospitalized patients and their families better-understood diagnoses and treatments.
- Patients were more engaged in their care, and compliance improved
After the success of the randomized trial, the Frankel Cardiovascular Center at the University of Michigan Health System adopted the program for all its inpatient units and outpatient facilities.
There it is – an example of what Christensen says disruptive innovation is – small, simple changes in specific areas. That is where stakeholders are engaged, quality and safety are protected, and change is sustainable.
The IHI and managing innovation
The IHI wants to know if disruptive innovation can safeguard quality and safety. In fact, their innovation management programs are trying to solve “stubborn intractable problems” with creative and productive thinking in a “dynamic learning environment.” It’s an effort to blend conservative approaches with revolutionary solutions. The proof is in the programming:
The American Medical Association Wants Alignment
Physicians and healthcare executives know that disruptive innovation is going to come from outside healthcare; that’s the nature of the beast. For example, a New England Journal of Medicine survey showed that a majority of healthcare leaders (65%) believe that the most promising innovation in primary care will come from start-ups.
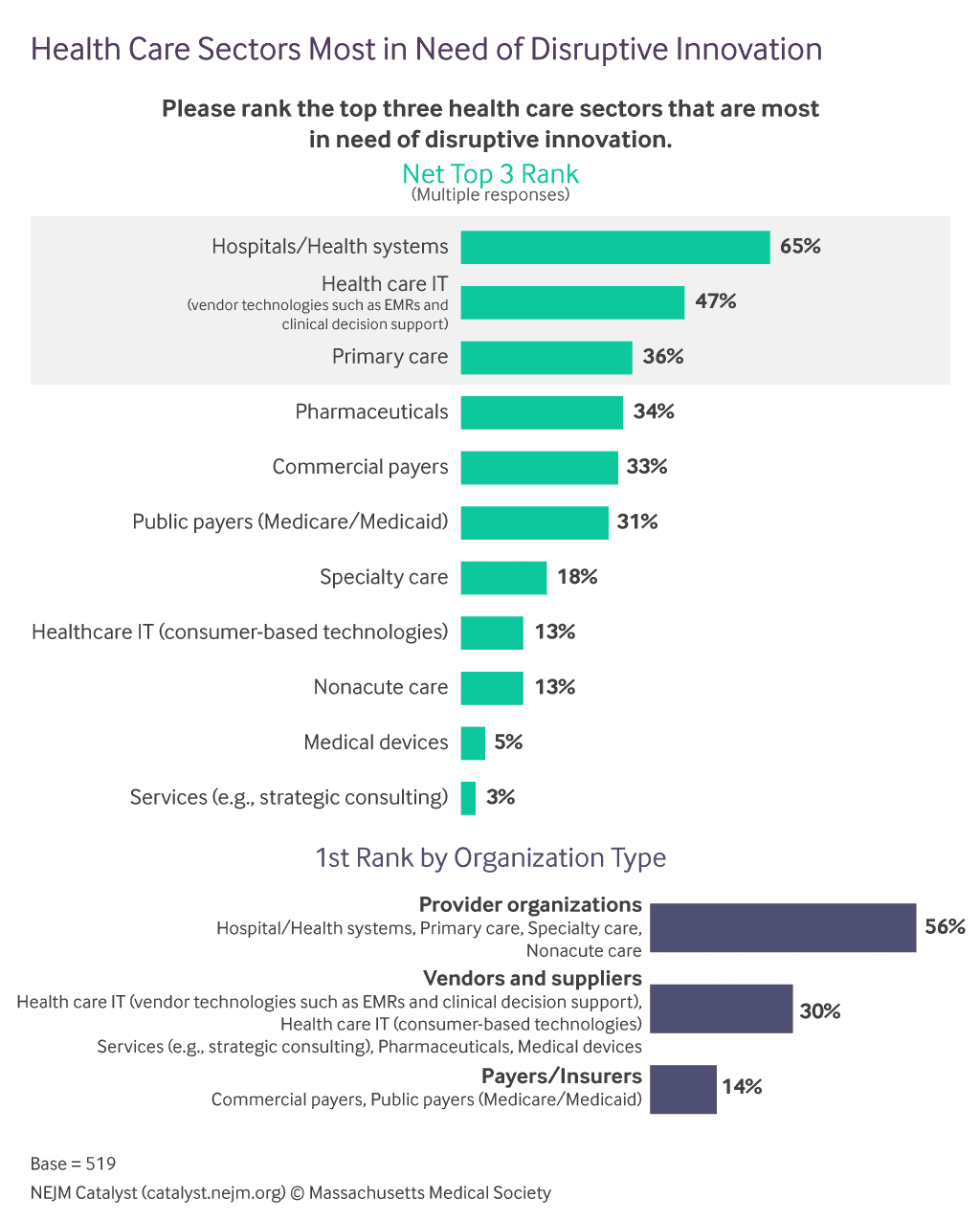 From NEJM Catalyst’s New Marketplace Survey: The Sources of Health Care Innovation, https://catalyst.nejm.org/disruptive-innovation-in-healthcare-survey/, February 16, 2017.
From NEJM Catalyst’s New Marketplace Survey: The Sources of Health Care Innovation, https://catalyst.nejm.org/disruptive-innovation-in-healthcare-survey/, February 16, 2017.
However, it still needs to be managed to ensure it addresses quality and patient safety. It’s safe to say that the American Medical Association (AMA) has had it with innovations developed in isolation from healthcare, like electronic medical records. As a result, the AMA has created several different initiatives to facilitate physician’s influence and collaboration with the development of digital solutions. Among them;
The Physician Innovation Network connects high tech companies and physicians so they can collaborate on innovative solutions to healthcare problems. Their goal is to “improve solutions.”
Perhaps the most comprehensive program to manage change is the AMA’s Integrated Health Model Initiative. It facilitates collaboration to ensure that technology solutions are developed with “real-world use and feedback.” For example, the group on Hypertension Management is discussing the potential and pitfalls of patient-generated health data. They are discussing new studies that indicate that Apple Watch and other wearable fitness devices may be able to detect hypertension. They are also sharing information on the benefits of mobile systems to support self-management of hypertension. These efforts are the steady beat of improvement and change at the street level of healthcare. They foster the type of innovation that meets the rigorous standards set by patient safety and quality.
We’ll say it again – innovation depends on simplicity. It makes adoption genetic. Healthcare is at its best when the million data points of information can be streamlined into a few insights and even fewer necessary actions. Remember the first core objective of the patient and provider adoption that we mentioned at the outset? And, the importance of changing behaviors that affect outcomes? Notepads and Apple watches meet that bar. It might be unexpected that they are so small and unobtrusive, but the best innovations are.
Healthcare wants innovation but isn’t ready
Innovation is disruption, but new technologies are necessary to reduce costs and improve care. Healthcare executives know that. They may be slow to adopt innovative ideas, but they also recognize that shrinking bottom lines and shifting patient volumes demand efficiencies that only new technologies can provide.
- 90 percent of healthcare chief strategy officers (CSOs) believe their industry will be transformed by new digital solutions in the next five years
- Only 13 percent of them believe their organizations are prepared for those changes
A technology tsunami is on the way. For those on the outside looking in, healthcare is the shining castle on the hill.
- 85 percent of technology companies and 77 percent of venture capitalists consider disrupting healthcare to be a top strategic priority
For those who think that disruption due to innovation is in full swing; think again. Accenture’s Disruptability Index indicates that healthcare’s current disruption score is the lowest of the 20 industries that it rates. However, it is the 9th most “susceptible to future disruption.” In other words – if you’re a healthcare decision maker brace yourself. Innovation, new technology and digital solutions promising to solve healthcare challenges are on the way. It’s going to take collaboration and a mile-high gauntlet to slow things down so you can make sense of it all.
Innovators who would try to scale the castle wall should be on notice. You must be able to prove that you can affect improvements to care and reduce costs without adversely impacting patient safety or quality.
When you think about highly regulated industries based on safety, the airline industry and healthcare are definitely at the top of the list. Both must innovate and grow without changing the basic foundation of what they do. Safety is their top priority.
- Planes must fly safely.
- Medicine must care for human beings safely.
The bottom line is that the airline industry is interested in innovation, but not if it impacts passenger safety. When they innovate, it is to improve the passenger experience, make security acuter, or streamline the flow of passengers. They do not innovate for innovation sake.
The same holds true in healthcare. Innovations that impact patient safety are not considered. Consequently, only new ideas, devices, and processes that improve patient safety, satisfaction and quality make the grade.
Innovation and medication adherence
One of the biggest risks to patient health and safety is medication adherence. It increases patient risk for adverse outcomes and directly impacts the quality of patient care. The statistics show the extent of the problem:
- In the United States, 3.8 billion prescriptions are written annually
- Approximately one in five new prescriptions are never filled
- Among those filled, approximately 50% are taken incorrectly, particularly about timing, dosage, frequency, and duration
- Direct health care costs associated with nonadherence have grown to approximately $100–$300 billion of U.S. health care dollars spent annually
The Centers for Disease Control and Prevention, (CDC) says that health IT can improve medication adherence. Studies have shown that electronic prescribing of medication increases “first-fill” medication adherence by 10 percent when compared to paper prescriptions.
Another enhancement to compliance is front-line, home-based remote monitoring like home blood pressure monitors. They improve medication adherence and prescribing as well. The CDC says that one physician group practice that employed these strategies improved its hypertension control rate from 68 percent in 2011 to 79 percent in 2014.
There are other innovative ways to improve medication adherence.
Wireless pill bottles have cellular chips and sensors embedded in the bottle. These are especially important for specialty treatments like cancer drugs. The chip collects data on when the patient takes the drug and if a dose is missed. It analyzes the information, posts it on a secure dashboard and alerts the pharmacist, patient or his or her caregiver. One manufacturer reports that the wireless pill bottle improved adherence by as much as 20 percent and increased the length of time that the patient stayed on the therapy by up to 30 percent.
A CDC Grand Rounds paper echoed these findings. It said that there are several successful strategies to improve medication adherence and one of them is “the use of health information technology tools to improve decision-making and communication during and after office visits.”
The future of innovation
Innovators will innovate and not always with an understanding of healthcare. Providers will provide care in the best way they know how; through evidence-based medicine. Friction between the two will continue. Only communication and collaboration will allow innovation to be adopted for the benefit of patients, the improvement of quality and safety, and the reduction of cost. The rapid-fire development of yet another new technology will get nowhere without the involvement of the healthcare community.
It may be hard to believe, but the old stalwarts, the AHRQ and the IHI, may be paving the road for this to happen. They may be the ones who can teach the two sides to collaborate, think together, brainstorm together, and craft technology that is eminently applicable to the daily delivery of healthcare in myriad settings. Whether it’s a trauma center or a physician’s practice, we need advances; we just need the ones that work.
Like the airline industry, healthcare isn’t looking to reinvent the wheel. They are looking to make it more efficient, faster, less expensive and more effective for those who use it. Innovators need to realize this and open up a dialogue with those who they would serve. The point is not to create a million new widgets. It’s to create the best ones with insight, collaboration, and a detailed understanding of the user’s needs and priorities.
William Payne, MD is an orthopedic surgeon, healthcare executive and entrepreneur. He is a co-founder and CEO of myowndoctor.com, a telemedicine platform that helps providers virtualize care, educate their patients and caregivers, and coordinate with care teams. He believes that telemedicine can cut through the current chaotic healthcare dynamic and create a delivery system that exponentially increases access and results in quality healthcare delivery for all.
